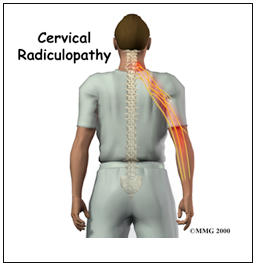
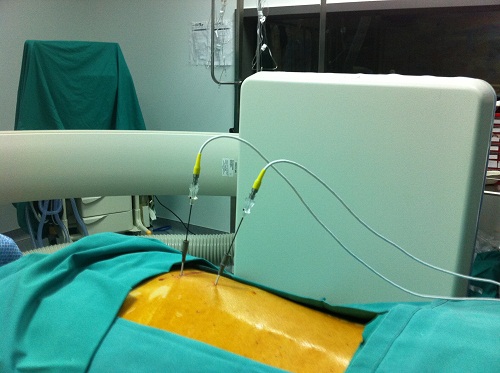
Cervical radicular pain is the pain caused by irritation or inflammation or injury of a cervical spine nerve. The pain is located in the upper arm ipsilateral to the lesion and is acute, stabbing, electric shock-like. (3,4)
Cervical radicular pain has to be differentiated from cervical radiculopathy. In radiculopathy there is objective sensory or/and motor loss. These two entities should not be confused, as it usually happens. Radicular pain is a symptom induced by ectopic excitation, while radiculopathy involves also neurological signs, such as sensory or/and motor changes. The two disorders may co-exist and have the same causes, e.g. intervertebral foraminal stenosis, disc herniation, infection and other inflammatory conditions. There is also the case of patients initially suffering from radiculitis (nerve root inflammation) that later on progresses into radiculopathy.
Cervical Radiculopathy
CAUSES
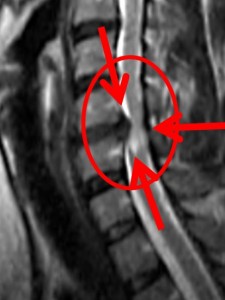
The most common cause of acute and subacute (6-12 weeks) cervical radicular pain is cervical disc herniation .
The most common cause of chronic (over 3 months) cervical radicular pain is the formation of adhesions around a nerve root and its chronic irritation. Adhesions may form as a result of acute inflammation due to disc herniation or after spine surgery.
Other causes may be: spinal canal stenosis, intervertebral foraminal stenosis (at the point where the nerve root exits), spondylolysthesis, syringomyelia and radiculitis following radiation or chemotherapy.
DIAGNOSIS
Cervical radicular pain is characterized by neck pain radiating to the posterior side of the shoulder, forearm and sometimes may reach down to the hand. Radiating pain follows the dermatome distribution of the affected nerve but also affects the tissues innervated by this nerve, such as muscles, joints, ligaments and skin. (4,9)
Pain originating from the fourth cervical root (C4) is localized in the neck and suprascapular region. Pain from the fifth cervical root (C5) radiates to the forearm, whereas pain from the sixth and seventh root (C6 and C7) extends to the neck, shoulder, forearm and hand.
PHYSICAL EXAMINATION
The diagnosis is based on the history, clinical examination and supplementary tests. The classical neurological examination includes sensory, motor and reflex examination.
 There are a number of special clinical tests relating to the diagnosis of cervical radicular pain:
There are a number of special clinical tests relating to the diagnosis of cervical radicular pain:
1. Spurling test. With patient’s neck in extension and head turned to the side of the painful shoulder, the clinician exerts vertical pressure on the head. Induced shoulder or forearm pain is an indication of probable compression of the cervical spinal root.
2. Shoulder adduction test. The patient elevates the arm above the head. Reduction or elimination of pain indicates probable cervical radicular origin.
Shoulder adduction test. The patient elevates the arm above the head. Reduction or elimination of pain indicates probable cervical radicular origin.
3. 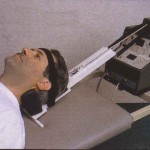 Vertical head traction test. The patient lies on the back and the clinician exerts vertical head traction equal to about 10-15 kilos. Reduction or elimination of pain indicates probable cervical radicular origin.
Vertical head traction test. The patient lies on the back and the clinician exerts vertical head traction equal to about 10-15 kilos. Reduction or elimination of pain indicates probable cervical radicular origin.
| INTERVERTEBRAL LEVEL |
NERVE ROOT |
PAIN DISTRIBUTION |
MUSCLE WEAKNESS |
SENSORY LOSS |
REFLEX LOSS |
| C4-C5 | C5 | MEDIAL SCAPULA
LATERAL UPPER ARM DOWN TO ELBOW |
DELTOID
SUPRASPINATUS INFRASPINATUS |
LATERAL UPPER ARM |
SUPINATOR REFLEX |
| C5-C6 | C6 | LATERAL FOREARM
THUMB AND FOREFINGER |
BICEPS BRANCHIALIS BRACHIORADIALIS WRIST EXTENSORS |
THUMB AND FOREFINGER |
BICEPS REFLEX |
| C6-C7 | C7 | MEDIAL SCAPULA
POSTERIOR UPPER ARM DORSAL FOREARM AND THIRD FINGER |
TRICEPS
WRIST FLEXORS EXTENSOR DIGITORUM |
POSTERIOR FOREARM
THIRD FINGER |
TRICEPS REFLEX |
| C7-T1 | C8 | SHOULDER
ULNAR PART OF FOREARM FIFTH FINGER |
THUMB FLEXOR |
FIFTH FINGER |
From Carette S and Fehlings MG
SUPPLEMENTARY EXAMINATIONS
The most commonly used supplementary examinations are radiological evaluation, electrophysiological testing and diagnostic selective nerve root blocks. Plain X-ray examinations are used mainly to rule out other serious primary pathology, such as tumor, infection and vertebral fracture.
CT scan provides good information on bone structures but there are limitations with regard to soft tissues. MRI is the examination of choice, showing morphological changes taking place in intervertebral discs, spinal cord, nerve roots and surrounding soft tissues. The diagnosis should not be based only on radiological findings, as a number of studies have shown that approximately 30% of patients with MRI findings are asymptomatic. When clinical and radiological findings match, then it is much easier to make a proper diagnosis. (6,12,13)
2 . ELECTROPHYSIOLOGICAL TESTS
Electrophysiological tests include nerve conduction and electromyography (EMG). These are useful when there is suspicion for nerve defect but they do not provide any particular information regarding pain.
3. DIAGNOSTIC SELECTIVE NERVE ROOT BLOCKS
These are applied when there is doubt about which specific nerve root causes the pain. With this technique, the nerve root is blocked with 0,5ml local anaesthetic and then the patient has to report whether his/her pain impoves at least by 50%. Every suspicious nerve root is blocked separately in different sessions until the one causing the pain is identified. (15)
DIFFERENTIAL DIAGNOSIS
Before setting the final diagnosis, it is imperative to investigate and exclude any other serious primary pathology, such as tumor, infection and vertebral fracture.
A tumor causing brachial pain of neuropathic type is the Pancoast tumor, which is an apical lung tumor that may compress the subclavian artery, phrenic nerve, brachial plexus and sympathetic ganglion, causing the so-called Horner syndrome. Metastases from some primary condition in the cervical spine may also cause brachial pain.
The clinical examination and history should be also used to rule out any probable pathology of the shoulder and cervical facet joints. Shoulder pain limits only the shoulder motion, while the cervical facet joint syndrome restricts the neck rotational movements. There is also increased sensitivity on paravertebral pressure and pseudoradicular pain radiating to the shoulder. (16)
TREATMENT
Α. CONSERVATIVE TREATMENT (6,17,18,19)
For the treatment of acute and subacute condition, anti-inflammatory drugs are recommended but only for a short period to avoid potential severe cardiovascular and gastrointestinal complications that might occur.
The chronic condition is treated with drugs administered in neuropathic pain, such as antidepressants (amitriptyline), antiepileptics (carbamazepine, oxcarbazepine, gabapentin, pregabalin). Although there are not yet studies establishing their efficacy in cervical radicular pain, this pain falls in the category of neuropathic pain and drugs mentioned above are definitely indicated.
In case of resistant pain to therapy, mild opioids may be added, such as codeine and tramadol.
In one of Cochrane’s reviews, the value of spinal traction application was evaluated in the treatment of cervical pain with or without radicular pain and , as regards the efficacy of the method, there was no evidence either to support or reject it.
Multifactorial rehabilitation is recommended with physical therapy and chiropractic manipulations.
In case pain persists or the patient does not tolerate the potential adverse events of drugs that s/he should take on a long-term basis and before deciding to administer any strong opioids, it is recommended to apply innterventional pain therapies.
Before starting pharmaceutical treatment on a long-term basis, many patients choose a minimally invasive therapy which intervenes straight to the origin of pain, in order to avoid chronic addiction to drugs with several side effects. In many cases, the ideal treatment is achieved with combination of pharmacotherapy and interventional techniques.
Percutaneous Cervical Disc Nucleoplasty
INTERVENTIONAL PAIN TREATMENT
1. Epidural Corticosteroid Injection (21,22,23,30,31,32,33)
When the disease is in its acute or subacute form, cervical epidural corticosteroid injection is indicated. The technique used, is the posterior translaminar approach, whereas the transforaminal epidural injection is avoided due to high risk of severe complications, as opposed to the lumbar spine where the transforaminal approach is preferred.
Systematic research worldwide leads to the conclusion that the cervical epidural corticosteroid injection is significantly effective in the treatment of acute and subacute cervical radicular pain and should always be applied before surgery decision.
2. Neuroplasty (adhesiolysis) with Racz catheter
When the disease is in its chronic form -as it usually happens after spine surgery or following the acute and subacute phase of radiculitis from disc herniation that had been undertreated with conservative therapy- neuroplasty (adhesiolysis) with Racz catheter is indicated.
The American Society of Interventional Pain Physicians (ASIPP) published evidence-based guidelines for invasive techniques in the management of chronic spinal pain.
According to these guidelines, there is strong evidence indicating the efficacy of neuroplasty with corticosteroids in the short and long-term control of pain in refractory radiculopathy and neuropathic spinal pain.
3. Pulsed Radiofrequency Therapy (PRF)
Randomized controlled studies have demonstrated the efficacy of PRF applied on the dorsal spinal root ganglion (DRG) of the cervical spine. According to evidence-based medicine, the application of the method in cases of chronic cervical radiculitis is strongly recommended.
The duration of analgesia varies from case to case. The technique is safe and can be repeated as many times as needed. If, despite the repetitive therapeutic sessions with pulsed radiofrequency the result has limited duration, then conventional radiofrequency can be applied. This application, however, destroys (ablates) the ganglion and may cause slight muscle weakness in the arm.(59,60,61)
4. Spinal Cord Stimulation(65)
It is a neuromodulatory therapy, which is used in case all other less invasive methods fail. Its efficacy in treating chronic resistant neuropathic pain is significant.
C. SURGICAL TREATMENT
Surgery is indicated in case the spinal cord is severely compressed with high risk of causing myelopathy with permanent severe irreversible neurological impairment.
In a randomized study, comparison was made between surgical and conservative treatment and it was found that there was substantial improvement in pain 3 months postoperatively. However, one year later there was no difference between the two patient groups. A small randomized study demonstrated that there are no differences in the neurologic outcome between patients who were treated surgically or conservatively.
Thus, surgical operation should be limited only to those patients whose neurological condition is so aggravated that the patient is in risk for permanent irreversible neurologic impairment.
MEDICAL INFORMATION SOURCES
1. PAIN PRACTICE JOURNAL
2. BONICA”S MANAGEMENT OF PAIN
3. PAIN PHYSICIAN JOURNAL
4. INTERVENTIONAL PAIN MANAGEMENT BOOK
5. NEUROMODULATION JOURNAL
LITERATURE
1. Guyatt G, Gutterman D, Baumann MH, et al.
Grading strength of recommendations and quality of evidence
in clinical guidelines: report from an american college of chest
physicians task force. Chest. 2006;129:174–181.
2. van Kleef M, Mekhail N, Van Zundert J. Evidencebased
guidelines for interventional pain medicine according to
clinical diagnoses. Pain Pract. 2009;9:247–251.
3. Rathmell JP, Aprill C, Bogduk N. Cervical transforaminal
injection of steroids. Anesthesiology. 2004;100:1595–
1600.
4. Bogduk N. Medical Management of Acute Cervical
Radicular Pain: and Evidence-based Approach. 1st ed. Newcastle,
Australia: The Newcastle Bone and Joint Institute;
1999.
5. Merskey H, Bogduk N. Classification Descriptions
of Chronic Pain Syndromes and Definitions of Pain Terms.
2nd ed. Seattle, WA: IASP Press; 1994.
6. Van Zundert J, Harney D, Joosten EA, et al. The role
of the dorsal root ganglion in cervical radicular pain: diagnosis,
pathophysiology, and rationale for treatment. Reg Anesth
Pain Med. 2006;31:152–167.
7. Radhakrishnan K, Litchy WJ, O’Fallon WM,
Kurland LT. Epidemiology of cervical radiculopathy. A
population-based study from Rochester, Minnesota, 1976
through 1990. Brain. 1994;117(Pt 2):325–335.
8. Sluijter ME. Radiofrequency Part I. Meggen, Switzerland:
Flivopress. 2001.
9. Slipman CW, Plastaras CT, Palmitier RA, Huston
CW, Sterenfeld EB. Symptom provocation of fluoroscopically
guided cervical nerve root stimulation. Are dynatomal
maps identical to dermatomal maps? Spine. 1998;23:2235–
2242.
10. Fager CA. Identification and management of radiculopathy.
Neurosurg Clin N Am. 1993;4:1–12.
11. Carette S, Fehlings MG. Clinical practice. Cervical
radiculopathy. N Engl J Med. 2005;353:392–399.
12. Boden SD, McCowin PR, Davis DO, Dina TS, Mark
AS, Wiesel S. Abnormal magnetic-resonance scans of the cervical
spine in asymptomatic subjects. A prospective investigation.
J Bone Joint Surg Am. 1990;72:1178–1184.
13. Teresi LM, Lufkin RB, Reicher MA, et al.
Asymptomatic degenerative disk disease and spondylosis of
the cervical spine: MR imaging. Radiology. 1987;164:83–
88.
14. Voerman VF, van Egmond J, Crul BJ. Elevated detection
thresholds for mechanical stimuli in chronic pain patients:
support for a central mechanism. Arch Phys Med Rehabil.
2000;81:430–435.
15. Anderberg L, Saveland H, Annertz M. Distribution
patterns of transforaminal injections in the cervical spine
evaluated by multi-slice computed tomography. Eur Spine J.
2006;15:1465–1471.
16. Mumenthaler M, Mattle H. Intervertabral disk
disease as a cause of radicular syndromes. In: Mumenthaler
M, Mattle H, eds. Neurology. 4th ed (revised and enlarged).
Stuttgart, Germany and New York: Georg Thieme Verlag;
2004;728–738.
17. Haines T, Gross A, Burnie SJ, Goldsmith CH, Perry
L. Patient education for neck pain with or without radiculopathy.
Cochrane Database Syst Rev. 2009;1:CD005106.
18. Graham N, Gross A, Goldsmith CH, et al. Mechanical
traction for neck pain with or without radiculopathy.
Cochrane Database Syst Rev. 2008;3:CD006408.
19. Persson LC, Lilja A. Pain, coping, emotional state
and physical function in patients with chronic radicular neck
pain. A comparison between patients treated with surgery,
physiotherapy or neck collar—a blinded, prospective randomized
study. Disabil Rehabil. 2001;23:325–335.
20. Abdi S, Datta S, Trescot AM, et al. Epidural steroids
in the management of chronic spinal pain: a systematic review.
Pain Physician. 2007;10:185–212.
21. Stav A, Ovadia L, Sternberg A, Kaadan M, Weksler
N. Cervical epidural steroid injection for cervicobrachialgia.
Acta Anaesthesiol Scand. 1993;37:562–566.
22. Castagnera L, Maurette P, Pointillart V, Vital JM,
Erny P, Senegas J. Long-term results of cervical epidural
steroid injection with and without morphine in chronic cervical
radicular pain. Pain. 1994;58:239–243.
23. Peloso P, Gross A, Haines T, Trinh K, Goldsmith
CH, Burnie S. Medicinal and injection therapies for mechanical
neck disorders. Cochrane Database Syst Rev. 2007;
3:CD000319.
24. Benyamin RM, Singh V, Parr AT, Conn A, Diwan S,
Abdi S. Systematic review of the effectiveness of cervical epidurals
in the management of chronic neck pain. Pain Physician.
2009;12:137–157.
25. Pasqualucci A, Varrassi G, Braschi A, et al. Epidural
local anesthetic plus corticosteroid for the treatment of cervical
brachial radicular pain: single injection versus continuous
infusion. Clin J Pain. 2007;23:551–557.
4. Cervical Radicular Pain • 15
26. Rowlingson JC, Kirschenbaum LP. Epidural analgesic
techniques in the management of cervical pain. Anesth
Analg. 1986;65:938–942.
27. Ferrante FM, Wilson SP, Iacobo C, Orav EJ, Rocco
AG, Lipson S. Clinical classification as a predictor of therapeutic
outcome after cervical epidural steroid injection. Spine.
1993;18:730–736.
28. Grenier B, Castagnera L, Maurette P, Erny P,
Senegas J. [Chronic cervico-brachial neuralgia treated by cervical
epidural injection of corticosteroids. Long-term results].
Ann Fr Anesth Reanim. 1995;14:484–488.
29. Cicala RS, Westbrook L, Angel JJ. Side effects and
complications of cervical epidural steroid injections. J Pain
Symptom Manage. 1989;4:64–66.
30. Abbasi A, Malhotra G, Malanga G, Elovic EP, Kahn
S. Complications of interlaminar cervical epidural steroid
injections: a review of the literature. Spine. 2007;32:2144–
2151.
31. Anderberg L, Annertz M, Persson L, Brandt L, Saveland
H. Transforaminal steroid injections for the treatment of
cervical radiculopathy: a prospective and randomised study.
Eur Spine J. 2007;16:321–328.
32. Scanlon GC, Moeller-Bertram T, Romanowsky SM,
Wallace MS. Cervical transforaminal epidural steroid injections:
more dangerous than we think? Spine. 2007;32:1249–
1256.
33. Malhotra G, Abbasi A, Rhee M. Complications of
transforaminal cervical epidural steroid injections. Spine.
2009;34:731–739.
34. Lee JH, Lee JK, Seo BR, Moon SJ, Kim JH, Kim SH.
Spinal cord injury produced by direct damage during cervical
transforaminal epidural injection. Reg Anesth Pain Med.
2008;33:377–379.
35. Lee JY, Nassr A, Ponnappan RK. Epidural
hematoma causing paraplegia after a fluoroscopically guided
cervical nerve-root injection. A case report. J Bone Joint Surg
Am. 2007;89:2037–2039.
36. Brouwers PJ, Kottink EJ, Simon MA, Prevo RL. A
cervical anterior spinal artery syndrome after diagnostic
blockade of the right C6-nerve root. Pain. 2001;91:397–399.
37. Rosenkranz M, Grzyska U, Niesen W, et al. Anterior
spinal artery syndrome following periradicular cervical nerve
root therapy. J Neurol. 2004;251:229–231.
38. Ludwig MA, Burns SP. Spinal cord infarction following
cervical transforaminal epidural injection: a case report.
Spine. 2005;30:E266–E268.
39. McMillan MR, Crumpton C. Cortical blindness and
neurologic injury complicating cervical transforaminal injection
for cervical radiculopathy. Anesthesiology. 2003;99:509–
511.
40. Rozin L, Rozin R, Koehler SA, et al. Death during
transforaminal epidural steroid nerve root block (C7) due to
perforation of the left vertebral artery. Am J Forensic Med
Pathol. 2003;24:351–355.
41. Tiso RL, Cutler T, Catania JA, Whalen K. Adverse
central nervous system sequelae after selective transforaminal
block: the role of corticosteroids. Spine J. 2004;4:468–474.
42. Beckman WA, Mendez RJ, Paine GF, Mazzilli MA.
Cerebellar herniation after cervical transforaminal epidural
injection. Reg Anesth Pain Med. 2006;31:282–285.
43. Ziai WC, Ardelt AA, Llinas RH. Brainstem stroke
following uncomplicated cervical epidural steroid injection.
Arch Neurol. 2006;63:1643–1646.
44. Suresh S, Berman J, Connell DA. Cerebellar and
brainstem infarction as a complication of CT-guided transforaminal
cervical nerve root block. Skeletal Radiol. 2007;
36:449–452.
45. Ruppen W, Hugli R, Reuss S, Aeschbach A, Urwyler
A. Neurological symptoms after cervical transforaminal injection
with steroids in a patient with hypoplasia of the vertebral
artery. Acta Anaesthesiol Scand. 2008;52:165–166.
46. Muro K, O’Shaughnessy B, Ganju A. Infarction of
the cervical spinal cord following multilevel transforaminal
epidural steroid injection: case report and review of the literature.
J Spinal Cord Med. 2007;30:385–388.
47. Gillilan LA. The arterial blood supply of the human
spinal cord. J Comp Neurol. 1958;110:75–103.
48. Bruneau M, Cornelius JF, Marneffe V, Triffaux M,
George B. Anatomical variations of the V2 segment of the
vertebral artery. Neurosurgery. 2006;59:ONS20–ONS24; discussion
ONS-24.
49. Huntoon MA. Anatomy of the cervical intervertebral
foramina: vulnerable arteries and ischemic neurologic injuries
after transforaminal epidural injections. Pain. 2005;117:104–
111.
50. Narouze S. Ultrasonography in pain medicine: a
sneak peak at the future. Pain Pract. 2008;8:223–225.
51. Karasek M, Bogduk N. Temporary neurologic deficit
after cervical transforaminal injection of local anesthetic. Pain
Med. 2004;5:202–205.
52. Benzon HT, Chew TL, McCarthy RJ, Benzon HA,
Walega DR. Comparison of the particle sizes of different steroids
and the effect of dilution: a review of the relative
neurotoxicities of the steroids. Anesthesiology. 2007;106:331–
338.
53. Okubadejo GO, Talcott MR, Schmidt RE, et al.
Perils of intravascular methylprednisolone injection into the
vertebral artery. An animal study. J Bone Joint Surg Am.
2008;90:1932–1938.
54. Dreyfuss P, Baker R, Bogduk N. Comparative effectiveness
of cervical transforaminal injections with particulate
and nonparticulate corticosteroid preparations for cervical
radicular pain. Pain Med. 2006;7:237–242.
55. de Leon-Casasola OA. Transforaminal cervical epidural
injections. Reg Anesth Pain Med. 2008;33:190–191.
56. Van Zundert J, Huntoon M, van Kleef M. Transforaminal
cervical epidural steroid injections: time to stop?
Spine. 2009; in press.
16 • van zundert et al.
57. Owlia MB, Salimzadeh A, Alishiri G, Haghighi A.
Comparison of two doses of corticosteroid in epidural steroid
injection for lumbar radicular pain. Singapore Med J.
2007;48:241–245.
58. Van Zundert J, le Polain de Waroux B. Safety of
epidural steroids in daily practice: evaluation of more than
4000 administrations. In: Monitor TI, ed. XX Annual ESRA
Meeting. Rome, Italy: ESRA; 2000;122.
59. van Kleef M, Liem L, Lousberg R, Barendse G,
Kessels F, Sluijter M. Radiofrequency lesion adjacent to the
dorsal root ganglion for cervicobrachial pain: a prospective
double blind randomized study. Neurosurgery. 1996;38:
1127–1131; discussion 1131–1132.
60. Slappendel R, Crul BJ, Braak GJ, et al. The efficacy
of radiofrequency lesioning of the cervical spinal dorsal root
ganglion in a double blinded randomized study: no difference
between 40 degrees C and 67 degrees C treatments. Pain.
1997;73:159–163.
61. Van Zundert J, Patijn J, Kessels A, Lame I, van
Suijlekom H, van Kleef M. Pulsed radiofrequency adjacent to
the cervical dorsal root ganglion in chronic cervical radicular
pain: a double blind sham controlled randomized clinical trial.
Pain. 2007;127:173–182.
62. Cahana A, Van Zundert J, Macrea L, van Kleef M,
Sluijter M. Pulsed radiofrequency: current clinical and biological
literature available. Pain Med. 2006;7:411–423.
63. Persson LC, Carlsson CA, Carlsson JY. Long-lasting
cervical radicular pain managed with surgery, physiotherapy,
or a cervical collar. A prospective, randomized study. Spine.
1997;22:751–758.
64. Kadanka Z, Bednarik J, Vohanka S, et al. Conservative
treatment versus surgery in spondylotic cervical myelopathy:
a prospective randomised study. Eur Spine J. 2000;9:538–
544.
65. Melzack R, Wall PD. Pain mechanisms: a new
theory. Science. 1965;150:971–979.
66. Huntoon MA. Cervical spine: case presentation,
complications, and their prevention. Pain Med. 2008;9:S35–
S40.
67. Waldman SD. Interventional Pain Management.
Philadelphia, PA: Saunders, W.B.; 2001.
68. Larkin TM, Carragee E, Cohen S. A novel technique
for delivery of epidural steroids and diagnosing the level of
nerve root pathology. J Spinal Disord Tech. 2003;16:186–
192.
69. Racz GB, Heavner JE. Cervical spinal canal loculation
and secondary ischemic cord injury—PVCS—perivenous
counter spread—danger sign! Pain Pract. 2008;8:399–403