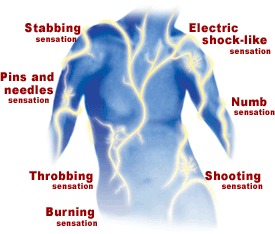
Neuropathic pain is defined as pain due to impairment or dysfunction of the peripheral or central nervous system. It is described by patients as “a burning, stabbing, tingling, electric-shock sensation” and is usually intense and continuous. It may coexist with nociceptive pain. It is resistant to therapy with painkillers, anti-inflammatory drugs, even opioids. It is not easy to diagnose and, when remaining untreated, it leads to limitation of physical activities, reduction of productivity, pessimism, depression, sleep disorders and isolation of the patient. For the identification and more effective management of pain, there is need for specialized medical treatment that is provided in Pain Clinics.
COMMON CONDITIONS – DISEASES INVOLVING NEUROPATHIC PAIN
- Trigeminal neuralgia
- Atypical prosopoalgia
- Post-herpetic neuralgia
- Diabetic polyneuropathy
- Stump pain after amputation
- Phantom-limb pain
- Multiple sclerosis
- Post-chemotherapy pain
- Post-irradiation pain
- HIV infection
- Alchoholism
- Cancer
- Nerve entrapment
- Postoperative neuropathy due to nerve injury
- Permanent sciatica following lower back surgery
- Other less common conditions
OTHER CHARACTERISTIC SYMPTOMS OF NEUROPATHIC PAIN
- Allodynia: pain induced by a stimulus which normally does not provoke pain. For example, a light touch on the face induces severe pain to the patient suffering from trigeminal neuralgia.
- Hyperalgesia : severe pain induced by a stimulus which would normally provoke only moderate discomfort
- Paraesthesia : abnormal sensation, e.g. pins-and-needles and tingling, without the existence of actual external stimuli provoking them
TREATMENT OF NEUROPATHIC PAIN
- Treatment of the aetiology itself when the causes are known and treatable. For example, strict control of blood glucose levels in patients with diabetes mellitus limits neuropathic pain symptoms. Unblocking some entrapped nerve usually stops neuropathic pain.
- Drugs:
1. Αntidepressants. They are administered for the treatment of neuropathic pain and are often proven to be effective. There are usually two groups of antidepressants: tricyclic antidepressants and serotonin & norepinephrine reuptake inhibitors (SNRIs). Selective serotonine reuptake inhibitors (SSRIs) are a third group of antidepressants that seem to have some effect, but they need further investigation. The increase of antidepressants dose should be done slowly in order to avoid or limit drug adverse events. Their action may take place within the first days or even after 4-6 weeks of slow increase of the dose. Some patients get quickly disappointed and wrongly discontinue the drug.
2. Αntiepileptics. They are administered to treat epilepsy but have also been found to reduce neuropathic pain. They are an alternative solution to antidepressants but can also be taken in combination with them when monotherapy is ineffective. Their action may start within the first few days or even after 4-6 weeks of slow increase of the dose. Some patients get quickly disappointed and wrongly discontinue the drug.
3. Tramadol. It acts as an agonist of opioid receptors and also inhibits serotonine and norepinephrin reuptake. This double action (action mechanism of opioid and antidepressant) limits the transmission of pain signals to the ascending and descending pain pathway. It has no anti-inflammatory action and has no noxious cardiovascular action. Special caution is needed with regard to dosage when administered in combination with antidepressants, due to the risk of inducing the serotonergic syndrome.
4. Opioids. They are not a drug of choice for neuropathic pain but they are administered when neuropathic pain is not effectively treated with the other therapeutic schemes and their combinations.
- CAPSAICIN PATCH. It is a new drug in the Greek market, with proven efficacy in a high rate of patients suffering from peripheral neuropathic pain.
- ALTERNATIVE MEDICINE– TENS. Acupuncture, relaxation therapies (massage, shiatsu etc), transcutaneous electric neurostimulation (TENS) may help to relieve patients from pain when applied in combination with the previously mentioned treatments.
- INTERVENTIONAL TREATMENTS
1. Pulsed radiofrequency applied to the posterior dorsal root ganglion (DRG)
2. Pulsed radiofrequency applied to the affected peripheral nerve
3. Peripheral nerve blocks with local anaesthetic and corticosteroid
5. Peripheral nerve stimulation
6. Surgical intervention depending on the aetiology of impairment (e.g. dissection of the affected peripheral nerve)
- PSYCHOLOGICAL SUPPORT THERAPIES. Pain may worsen with anxiety, stress and depression. On the contrary, the success rate of a therapy increases when the patient takes control of negative emotions, faces the problem with optimism and positive thinking and has reasonable expectations with regard to the therapeutic result.